 Larsen and collaborators highlight the fact that hypotonia and intellectual disability are common phenotypic features that may be more constant than the variable epilepsy phenotype. Also, there are wide differences in the severity of the epilepsy, ranging from milder focal seizures to epileptic spasms with hypsarrhythmia. On average, patients with SCN8A encephalopathy start having seizures at the age of 5 months, but the range of onset is very wide. 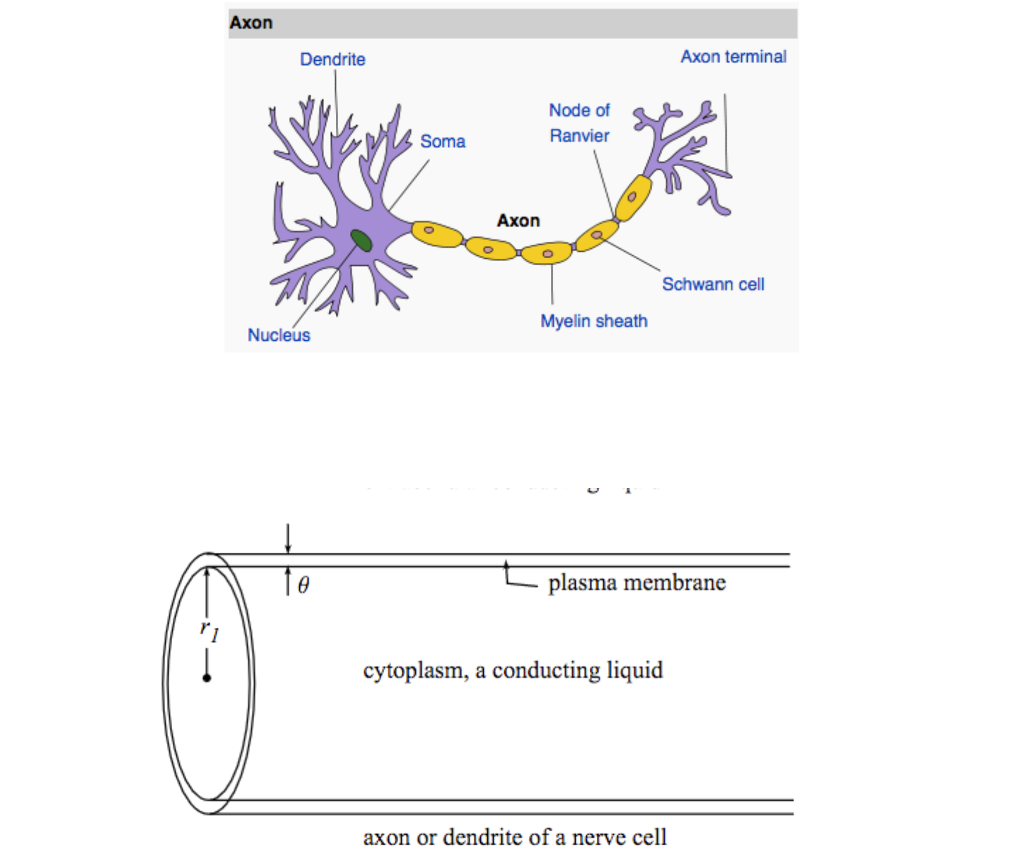
Spectrum of the SCN8A mutations identified by Larsen and collaborators. The publication by Larsen and collaborators now highlights the fact that epileptic encephalopathy is a common consequence of likely activating mutations. For SCN8A, the story was not clear for a long time. For SCN2A, likely gain-of-function mutations result in epileptic encephalopathy. These phenotypes are completely different to the epilepsy phenotypes due to gain-of-function. Loss-of-function mutations in SCN2A can lead to autism and intellectual disability, and loss-of-function mutations in SCN8A lead to intellectual disability and ataxia (OMIM 614306). First, what happens if the channel is less active, either due to a particular mutation or through a truncating mutation or deletion? For both SCN2A and SCN8A, these questions have been answered. Understanding the consequences of SCN2A and SCN8A mutations involves two opposite scenarios. Accordingly, changes in channel properties at the AIS can be far-reaching. It is at the AIS, where all the excitatory and inhibitory signals running up and down the neuron are integrated and where the decision is made whether the neuron will fire. Given the pivotal location of the AIS, it serves as the neuron’s main decision making center. Both ion channels are expressed at the axon initial segment ( AIS). In contrast to SCN1A, SCN2A and SCN8A channels are expressed on excitatory pyramidal cells. Basically, the neurons that are supposed to inhibit neuronal activity are reduced in their activity – resulting in too much excitation and epilepsy. 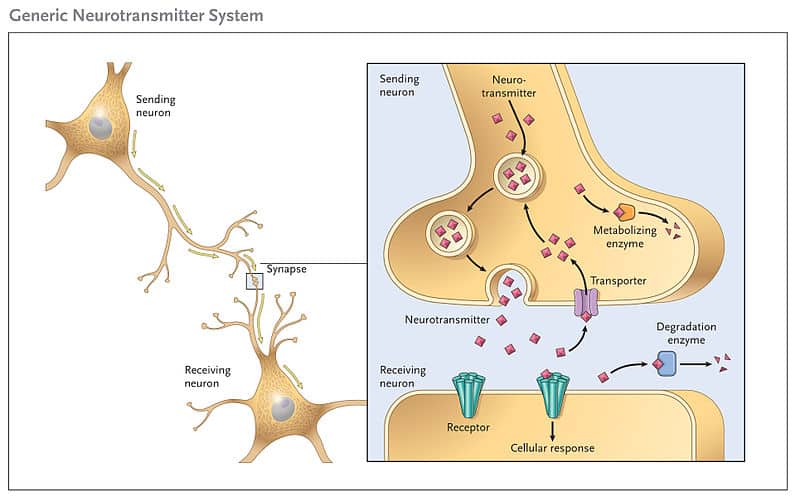
It is well accepted that in SCN1A-related Dravet Syndrome, lack of the sodium channel on inhibitory cells leads to decreased inhibition and net excitation. The SCN1A channel is mainly expressed on inhibitory interneurons, and lack of SCN1A, for example due to a truncating mutation, disruptive missense mutation, or deletion leads to the phenotype of Dravet Syndrome, a severe, fever-associated epileptic encephalopathy. 
SCN1A is by far the most common and best studied voltage-gated ion channel. Voltage-gated sodium channels allow for the influx of sodium into the cell upon a change of membrane potential – the ion channels are crucial for propagating the excitatory of inhibitory action of neurons along the dendrites, cell body, and axon. As of 2014, there are three voltage-gated sodium channel genes associated with severe human epilepsies, SCN1A, SCN2A, and SCN8A. For SCN2A and SCN8A, the mutations are assumed to be excitatory for KCNQ2, the mutations are thought to be dominant negative. Mutations in all three genes are now associated with severe epilepsies. The ion channels encoded by the SCN2A, SCN8A, and KCNQ2 genes are located at the axon initial segment, the part of the neuron where all excitatory and inhibitory impulses at the neuronal membrane are integrated and translated into an action potential. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
